0769-22660023
0769-22660023  0769-22660023
0769-22660023 First, the answer: If dry eye disease progresses to a severe stage, corneal transplant surgery may indeed be necessary.
Do you experience these symptoms daily?
After staring at a computer for an hour, your eyes feel dry as if covered in a haze. Blinking feels like fine sand grinding against your eyeballs, causing pain so intense you can't help but squint.
Scrolling through your phone for half an hour, only to see your whites instantly fill with red veins, itching so badly you want to rub them but dare not, as rubbing just makes them drier;
Spending an afternoon in an air-conditioned room, leaving your eyes sticky and dry, with even frequent use of “trendy eye drops” offering no relief;
Wearing contact lenses feels like a foreign object lodged in your eye, and after removal, the edges of your cornea turn red, blurring your vision so badly you can't even see the screen clearly...
These seemingly minor symptoms—dryness, itching, foreign body sensation—may be early warning signs of dry eye syndrome. If ignored or treated improperly over time, mild discomfort can progress to blurred vision, corneal damage, and even the risk of needing a corneal transplant.
Today, let's break down the science: Just how dangerous can this “minor” condition really be?
Image
First, understand:
Dry eye syndrome ≠ “lack of tears”—it's a “collapse of the tear film ecosystem”
Many mistakenly believe dry eye means “insufficient tears,” but that's incorrect!
Our eye surface is covered by a protective “tear film” composed of three layers:
Lipid layer (secreted by meibomian glands): Acts like “plastic wrap” to prevent rapid tear evaporation.
Aqueous layer: Functions as a “moisturizer” to hydrate the eye.
Mucous layer: Serves as an “adhesive” to anchor the tear film to the cornea.
Dry eye syndrome fundamentally stems from an imbalance in this “tear film ecosystem” — whether due to blocked meibomian glands causing “moisture retention failure,” insufficient blinking while screen-viewing accelerating tear evaporation, or inadequate mucin secretion leading to “tear film adhesion failure.”
Key takeaway: Dry eye syndrome manifests in 5 distinct types —
Image
Image
Don't underestimate it:
From “dry eyes” to “corneal transplant” may be just 3 steps away!
Image
Dry eye disease worsens silently. Many only panic when vision significantly declines, but by then, the optimal treatment window has long passed:
Step 1: Mild discomfort → Impacts quality of life
Early symptoms include dryness, foreign body sensation, and light sensitivity, especially noticeable in dry environments like air-conditioned rooms. Many choose to “tough it out,” but prolonged dryness leads to poor concentration, reduced reading efficiency, and disrupts daily work and life.
Step 2: Moderate Damage → Corneal Inflammation, Vision Loss
Without intervention, shortened tear film breakup time may cause corneal epithelial detachment, resulting in redness, stinging pain, and blurred vision. Abusing preservative-containing eye drops at this stage may further damage the ocular surface and trigger inflammation.
Step 3: Severe Crisis → Corneal Ulcers, Perforation, Requiring Transplantation
When meibomian glands become completely blocked, tear evaporation accelerates, leaving the cornea chronically dehydrated and prone to ulcers and perforation. At this stage, corneal transplantation is the only option to replace the diseased cornea, otherwise there is a risk of blindness.
Image
3 Deadly Misconceptions
That Are Accelerating Your Dry Eye Progression!
❌ Misconception 1: Relying on “Trendy Eye Drops” (Containing Borneol, Menthol, Vitamin B12)
Harm: These drops temporarily numb nerves with a “cooling sensation.” Long-term use damages the lipid layer of the tear film, worsening dryness. Preservative-containing drops—using one bottle is like soaking the cornea in preservatives—directly injure the corneal epithelium.
Correct Approach: Choose “preservative-free artificial tears” only for temporary hydration; they cannot replace treatment.
❌ Misconception 2: Hydrating without “sealing moisture”
Risk: Using artificial tears without restoring meibomian gland function is like adding water to an uncovered cup—it evaporates quickly, never solving the root issue.
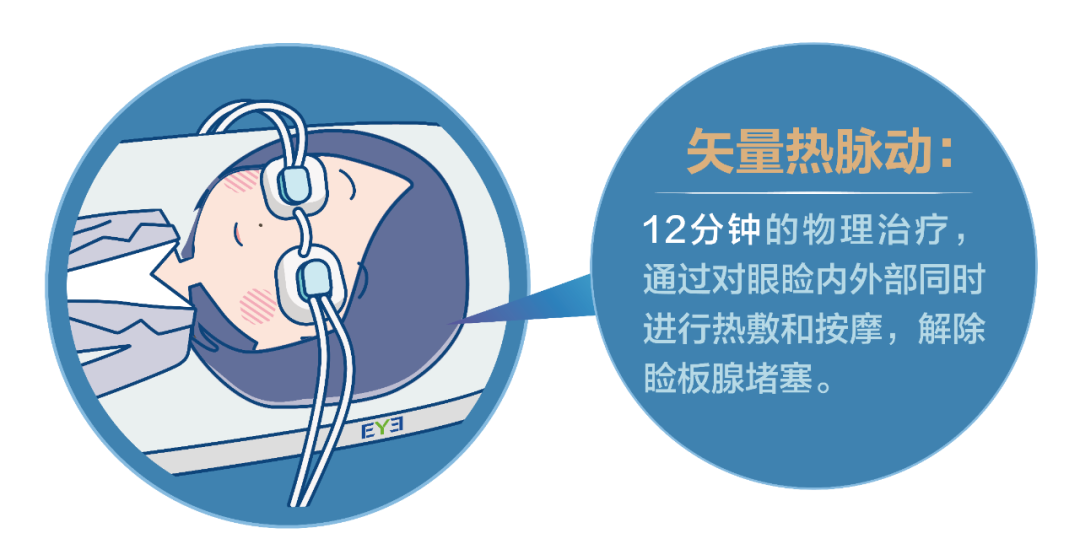
Correct approach: While hydrating, focus on repairing meibomian glands (e.g., through warm compresses and massage). This “covers the cup” to truly lock in moisture.
❌ Misconception 3: “If it can't be cured, why bother treating it?”
Risk: While dry eye syndrome cannot be “cured,” standardized treatment can fully control the condition and prevent worsening. Neglecting it means each “dry eye episode” causes “chronic damage” to the cornea.
Correct Approach: Early examination and intervention keep the condition mild, preventing corneal damage.
Image
Essential Guide:
4 Steps to Overcome Dry Eye Syndrome!
Image
1. Start with a “Comprehensive Ocular Surface Examination”: Visit a reputable ophthalmic institution for three core tests to determine the type and severity:
Tear Production Test: Measures how much tear fluid your eyes produce every 5 minutes;
Meibomian Gland Imaging: Assesses whether meibomian glands are blocked or atrophied;
Comprehensive Ocular Surface Analysis: Evaluates tear film breakup time (normal >14 seconds;<7 seconds indicates dry eye risk) and tear meniscus height (normal...